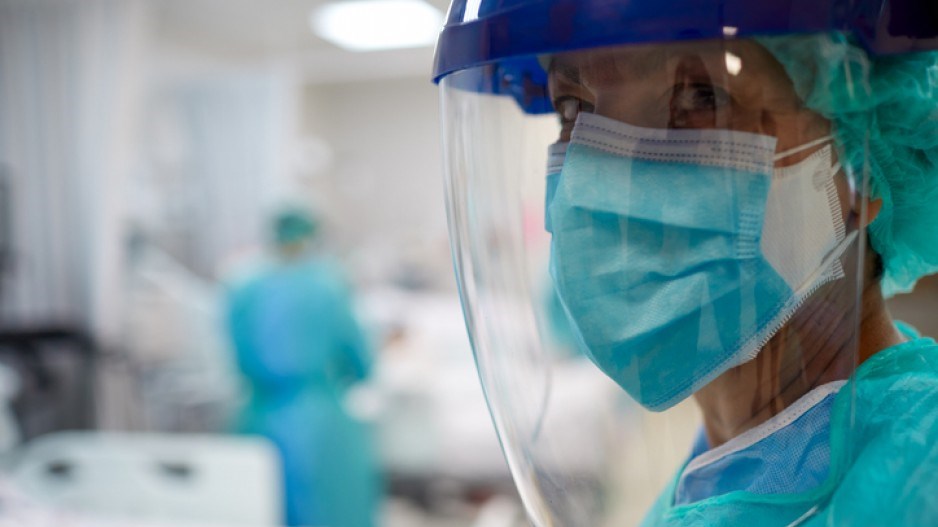
B.C.s frontline healthcare workers are reporting high levels of stress and burnout from the COVID-19 pandemic as case numbers continue to climb.
“COVID has only amplified nurses’ distress levels,” B.C. Nurses Union (BCNU) president Christine Sorensen said. “We have seriously ill nurses who need mental health support to be able to continue to support their patients.”
She said what nurses are dealing with at times approaches situations of “terror.”
She said they’re dealing with fear of infection while helping people dying in the absence of family members prohibited from deathbeds.
“The whole time, nurses are terrified of contracting COVID because they can’t access personal protective equipment (PPE),” Sorensen said. “It’s a really hard time for nurses.”
And, said Vancouver General Hospital intensive care unit nurse Cecilia Yeung, while health care operations do provide assistance, it is vital that health care workers do self-care, be aware of how their work is impacting their mental health and watch for signs of post-traumatic trauma.
“You’re exhausted,” Yeung said. “You don’t want to take anything home. You are constantly scrubbing yourself ‘til you are bleeding.”
“Socializing has been taken away,” she said. “Our lives are with COVID patients and home. We can’t go anywhere. We can’t de-stress.”
Indeed, nurses now face suicide ideation rates, plans or attempts two-three times higher than the national average, a new survey done by the BCNU and UBC has found. The survey is an update of one done in November 2019 and shows increased mental health issues.
All is cause for deep concern for Sorensen who wants to see greater government and employer transparency and significantly better reporting of statistics from WorkSafeBC.
The survey found some 41% are reporting several depression, 60% are emotionally exhausted and say they’re 57% experiencing high levels of burnout. The numbers are higher for acute care nurses.
Of those people, eight percent thought of committing suicide, three percent planned their death and one percent attempted to take their own lives.
What’s more, half of respondents scored within the positive range for post-traumatic stress disorder. Almost three-quarters scored within some level of anxiety, and 40% within the moderate to severe anxiety range. About the same numbers were found for depression.
About 60% indicated high emotional exhaustion, 32% feelings of high depersonalization, and 35% indicated feelings of low personal accomplishment.
Further, 24.1% had been told to work despite possible or confirmed virus exposure and 5.7% told to work despite having symptoms.
A survey done in June and July found 86% nurses concerned about contracting COVID in the workplace and 80% concerned about taking it home. Greater numbers of acute care and long-term care nurses were afraid of taking it home
Almost half said personal protective equipment was insufficient and 40% said it is critical to working effectively. Those numbers rise among long-term care nurses.
Among acute care and long-term care nurses, concerns about inadequate staffing were significantly higher than among nurses generally.
Further, 41% said respondents graded transparency around organizational pandemic decisions as poor or failing. Some 43% of acute care nurses felt that way.
“The majority of respondents (72%) reported that the average frequency of COVID-19 protocol and policy changes was weekly or higher. More than a quarter (27%) reported daily or higher,” the report said.
Moreover, the survey found higher levels of poor mental health around anxiety, depression, emotional exhaustion as well as negative treatment in the workplace and lower quality of nursing care.
Added to the stress of patient workloads, nurses report having to do clerical duties, obtain supplies and doing housekeeping duties.
Sorenson said nurses find themselves begging managers or security staff to unlock PPE supplies.
“Nurses don’t feel valued by the government of the employer,” she said. “They feel expendable.”
And, she asked the general public to move from banging pots and pans, calling nurses heroes, to heeding health care system calls for people to stay home, to protect themselves.
Doctors of B.C. president Dr. Kathleen Ross said all health care workers from cleaners to nurses and doctor are experiencing increased stress.
“Everyone’s working flat out to provide care,” Ross said. “Our capacity to keep working with these stress levels is not unlimited. We encourage physicians to speak to their peers and debrief wherever possible.”
Doctors of B.C. is also providing confidential assessments for those who request them, she said. “There are a number of peer-to-peer support groups that are running throughout the province. We want to be there for each other.”
For those on the job, Yeung said Ontario psychologist Dr. Melanie Joanisse’s Psychological First Aid for Frontline Health Care Providers During COVID-19: A Quick Guide to Wellness has been a welcome find.
And, Yeung is worried about the future effects of pandemic trauma nurses are witnessing.
“PTSD does not happen right away,” she said. “People are pushing through, pushing through. I worry some health care workers will experience some precursors of PTSD they don’t know about.”
“There’s a lot of professional help out there,” Yeung said. “Do self check-ins. It’s OK to feel a little off. You have to face it.”
As for WorkSafeBC, the province’s occupational health and safety regulator, Sorenson said transparency in reporting has declined in recent years. She said 26 nurses a month are assaulted in B.C.
“WorkSafe stopped reporting those statistics because we used them,” she said. “When you know how many nurses are injured, they pile up,” Sorenson said. “People don’t want the public to know how bad it is.”
And, she wants to see whistleblower protection laws extended to nurses. “They should be able to tell the public what is really going on.”
Further, Sorenson predicted, while nurses are committed to remaining at their posts through the pandemic, there could be a surge of departures from the profession once the threat ends. That, she said, is going to further compound an existing nursing shortage.
A response to the BCNU/UBC results from the Ministry of Health was expected.
@jhainswo